In Vitro Fertilization (IVF): Process, Advancements, and Patient Care
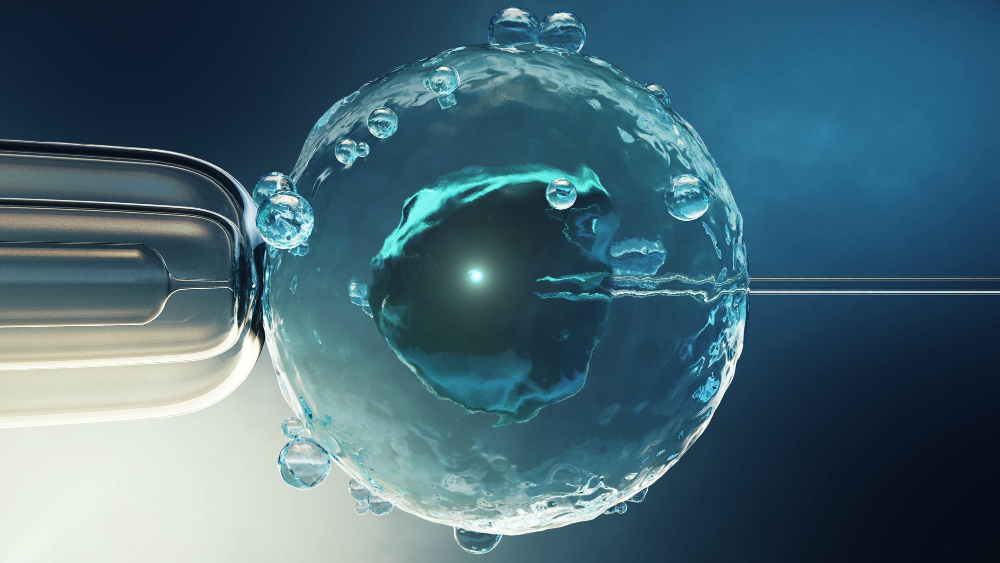
The landscape of reproductive medicine has undergone a profound transformation over the last several decades, offering unprecedented hope to individuals and couples facing infertility. At the forefront of Assisted Reproductive Technology (ART) is In Vitro Fertilization (IVF) Treatment, a complex and highly effective series of medical procedures designed to assist with the conception of a child. By facilitating the fertilization of an egg by a sperm outside the human body, medical professionals can bypass numerous biological barriers that prevent natural conception.
Medical Indications for IVF
Infertility is broadly defined as the inability to conceive after twelve months of regular, unprotected intercourse. However, the decision to pursue IVF is often based on specific, diagnosed medical conditions. Common indications for initiating this advanced reproductive treatment include:
- Fallopian Tube Damage or Blockage: Damaged or blocked fallopian tubes prevent the egg from traveling to the uterus and block the sperm from reaching the egg.
- Ovulation Disorders: Conditions such as Polycystic Ovary Syndrome (PCOS) or premature ovarian insufficiency can disrupt the regular release of eggs.
- Endometriosis: This condition occurs when tissue similar to the lining of the uterus grows outside of it, often affecting the function of the ovaries, uterus, and fallopian tubes.
- Male Factor Infertility: Below-average sperm concentration, poor mobility (motility), or abnormalities in sperm size and shape can severely impede natural fertilization.
- Unexplained Infertility: In some cases, despite comprehensive diagnostic evaluation, no identifiable cause for infertility is found.
The Step-by-Step IVF Protocol
The IVF process is meticulously timed and highly regulated, requiring close collaboration between patients, reproductive endocrinologists, and embryologists. The treatment cycle generally consists of five primary stages.
1. Ovarian Stimulation During a natural menstrual cycle, a woman typically produces a single mature egg. In an IVF cycle, the goal is to harvest multiple eggs to increase the chances of developing a viable embryo. Patients are prescribed injectable synthetic hormones, such as Follicle-Stimulating Hormone (FSH) and Luteinizing Hormone (LH), to stimulate the ovaries to produce multiple follicles. Throughout this phase, medical professionals monitor follicular development via transvaginal ultrasounds and track systemic hormone levels through frequent blood tests.
2. Egg Retrieval Once the follicles reach an optimal size, an injection of Human Chorionic Gonadotropin (hCG) is administered to trigger the final maturation of the eggs. Approximately 36 hours later, the egg retrieval procedure takes place. Under light sedation or anesthesia, a physician uses ultrasound guidance to insert a thin needle through the vaginal wall into the ovarian follicles, gently aspirating the follicular fluid and the microscopic eggs contained within.
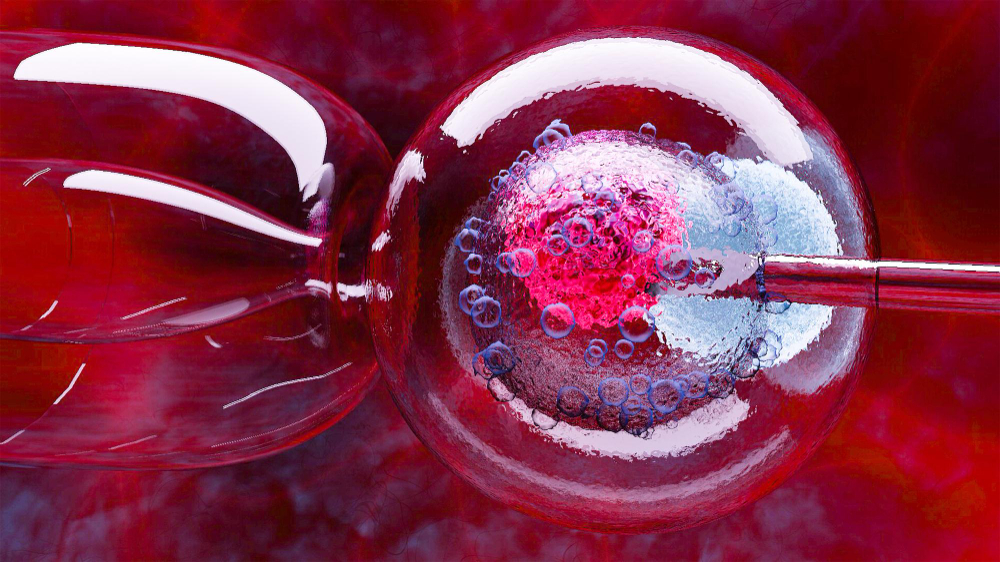
3. Sperm Collection and Fertilization Simultaneous with the egg retrieval, a semen sample is collected and processed in the andrology laboratory to isolate the most active and healthy sperm. The fertilization process can occur in two distinct ways. In conventional insemination, the healthy sperm and mature eggs are mixed and incubated together. However, if male factor infertility is a concern, embryologists utilize a specialized technique.
This technique, known as Intracytoplasmic Sperm Injection (ICSI), involves the direct injection of a single, highly viable sperm into the center of each mature egg, significantly increasing the probability of successful fertilization.
4. Embryo Culture Following successful fertilization, the resulting embryos are housed in specialized incubators that strictly mimic the environmental conditions of the human fallopian tube. Embryologists closely monitor their cellular division and developmental progression over the next three to five days. Embryos that reach the blastocyst stage (day five or six) often demonstrate higher implantation potential.
5. Embryo Transfer The final clinical step involves transferring one or more of the most viable embryos into the patient’s uterus. This is a minimally invasive procedure where a highly flexible, thin catheter is passed through the cervix. If an embryo successfully attaches to the uterine lining in the subsequent days, implantation occurs, resulting in a pregnancy. Any remaining high-quality embryos can be cryopreserved (frozen) for future use.
The Importance of Advanced Clinical Care
The success of reproductive treatments relies heavily on the technological capabilities of the embryology laboratory and the expertise of the clinical staff. High-tier medical institutions invest heavily in state-of-the-art incubation systems, stringent air quality control protocols within their laboratories, and advanced genetic testing capabilities like Preimplantation Genetic Testing (PGT). By choosing a highly accredited facility like Liv Hospital, patients ensure they are receiving care that aligns with the latest global standards in reproductive endocrinology, thereby maximizing their chances of a successful clinical outcome.
Beyond the rigorous clinical protocols and laboratory procedures, the journey through reproductive medicine requires an incredible amount of systemic resilience. The hormonal fluctuations, combined with the anticipation of treatment outcomes, underscore the necessity of comprehensive lifestyle support. Proper nutritional counseling, stress reduction techniques, and adequate psychological support are essential pillars that support the physical body during demanding medical treatments. Incorporating restorative daily practices can help individuals maintain systemic balance and emotional fortitude during complex medical journeys. To discover evidence-based strategies for integrating optimal wellness routines into daily life, patients and their families can explore the resources available at live and feel to nurture both physical and mental well-being.