Navigating the Path to Parenthood: A Comprehensive Guide to In Vitro Fertilization (IVF)
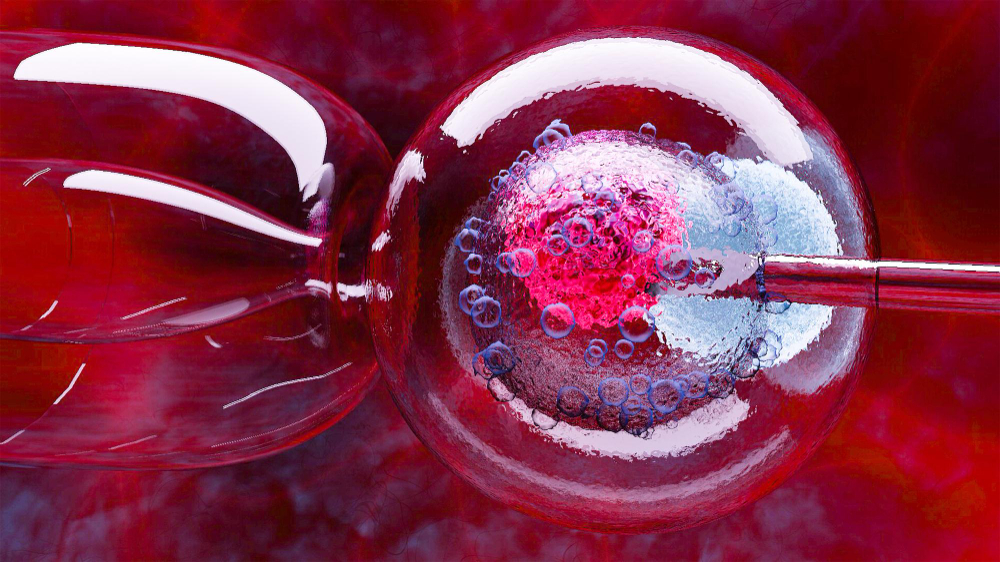
The journey to parenthood is a deeply profound experience, yet for millions of individuals worldwide, it presents unforeseen medical challenges. When natural conception proves difficult, modern reproductive medicine offers highly sophisticated solutions. At the forefront of Assisted Reproductive Technology (ART) stands In Vitro Fertilization (IVF) Treatment, a highly effective clinical intervention that has revolutionized the landscape of fertility care. By facilitating the union of an egg and sperm in a controlled laboratory environment, this advanced procedure bypasses numerous biological barriers, offering renewed hope to those facing complex reproductive obstacles. Understanding the physiological mechanisms, the detailed procedural steps, and the latest technological advancements associated with this treatment is essential for patients navigating the complexities of reproductive health.
Clinical Indications for IVF
The medical decision to initiate an IVF cycle is typically preceded by comprehensive diagnostic evaluations. Reproductive endocrinologists may recommend this clinical pathway for a variety of specific physiological conditions. One primary indication is tubal factor infertility, where fallopian tubes are damaged or completely blocked. This blockage prevents the natural transit of the egg to the uterus and inhibits sperm from successfully reaching the egg. Endometriosis, a condition characterized by the growth of endometrial-like tissue outside the uterine cavity, can also severely distort pelvic anatomy and impair natural fertility, frequently making IVF a necessary medical intervention.
Furthermore, male factor infertility plays a significant role in modern reproductive challenges. Conditions such as severe oligospermia (low sperm count), asthenozoospermia (poor sperm motility), or teratozoospermia (abnormal sperm morphology) can drastically reduce the probability of natural fertilization. In such instances, laboratory-assisted fertilization becomes indispensable. Additionally, patients facing ovulation disorders, premature ovarian insufficiency, or unexplained infertility—where no definitive biological cause can be identified despite exhaustive medical testing—often find success through these advanced reproductive protocols.
The IVF Process Step-by-Step
The clinical protocol for IVF is a meticulously orchestrated sequence of events, heavily reliant on precise physiological timing and continuous hormonal monitoring. The standard treatment cycle encompasses several distinct, critical phases designed to maximize the probability of a successful pregnancy.
1. Ovarian Stimulation and Monitoring In a natural, unmedicated menstrual cycle, the human body typically matures a single egg. However, to optimize the chances of generating a viable embryo, the IVF process requires the retrieval of multiple mature oocytes (eggs). Patients undergo a carefully managed regimen of injectable synthetic hormones, primarily Follicle-Stimulating Hormone (FSH) and Luteinizing Hormone (LH). These medications hyperstimulate the ovaries, prompting the simultaneous development of multiple ovarian follicles. Throughout this crucial phase, medical teams strictly monitor the patient’s physiological response through routine transvaginal ultrasounds to measure follicular growth and frequent blood tests to assess systemic estradiol levels.
2. Oocyte Retrieval Once the ovarian follicles reach optimum maturity, an injection of Human Chorionic Gonadotropin (hCG) or a specific agonist trigger is administered to induce the final maturation of the eggs. Exactly 36 hours post-trigger, the oocyte retrieval procedure is carefully performed.
Operating under intravenous sedation, a reproductive specialist utilizes advanced ultrasound guidance to pass a fine aspiration needle through the vaginal wall directly into the ovaries. The follicular fluid is carefully extracted, bringing the microscopic eggs with it into sterile collection tubes for immediate laboratory processing.
3. Sperm Preparation and Fertilization Concurrently with the egg retrieval, a semen sample is collected and processed in an advanced andrology laboratory. The sample undergoes strict washing and centrifugation protocols to isolate the most motile and morphologically normal sperm. Fertilization can then be achieved through two primary clinical methods. In conventional IVF, the prepared sperm and the retrieved eggs are co-incubated in a specialized culture medium, allowing natural penetration to occur.
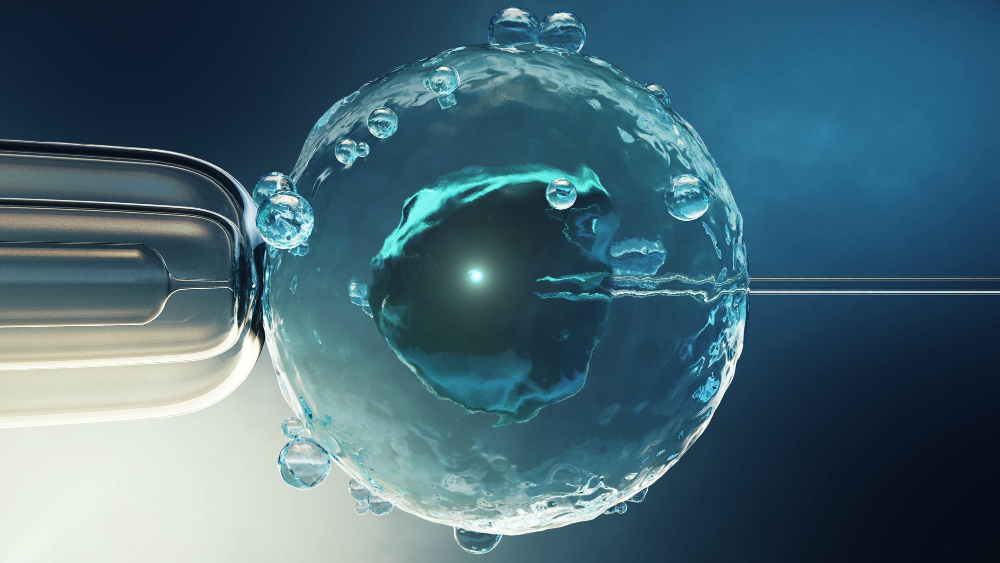
Conversely, in cases involving severe male factor infertility or previous fertilization failures, embryologists employ a highly specialized micromanipulation technique known as Intracytoplasmic Sperm Injection (ICSI). This method involves the direct injection of a single, carefully selected sperm into the cytoplasm of each mature egg, bypassing natural cellular barriers and significantly enhancing fertilization rates.
4. Embryo Culture and Development Following successful fertilization, the resulting zygotes are placed in state-of-the-art incubators that precisely replicate the physiological environment of the human fallopian tubes, strictly regulating temperature, humidity, and gas concentrations. Highly trained embryologists monitor the cellular division over a period of three to six days. The clinical goal is for the embryos to reach the blastocyst stage, a complex cellular structure comprising hundreds of cells, which generally demonstrates a much higher potential for successful uterine implantation.
5. Embryo Transfer and Cryopreservation The culminating phase of the active IVF cycle is the embryo transfer.
This minimally invasive procedure involves the loading of the selected embryo (or embryos) into a soft, highly flexible medical catheter. Under continuous ultrasound guidance, the physician carefully navigates the catheter through the cervix and deposits the embryo directly into the optimal region of the uterine lining. Following the transfer, patients typically receive luteal phase support in the form of progesterone supplementation to maintain an ideal physiological environment for implantation. Any remaining high-quality embryos that are not transferred can be cryopreserved using an ultra-rapid freezing technique called vitrification, preserving them indefinitely for potential future family-building efforts.
Advancements and Medical Excellence
The field of reproductive medicine is characterized by rapid, ongoing technological evolution. Modern IVF protocols frequently incorporate Preimplantation Genetic Testing (PGT), a sophisticated laboratory procedure that allows embryologists to screen embryos for chromosomal aneuploidies (an abnormal number of chromosomes) or specific monogenic hereditary disorders prior to transfer. This highly precise technology dramatically reduces the risk of recurrent implantation failure and early pregnancy loss. Achieving consistent, high success rates requires unparalleled laboratory standards and clinical expertise. Elite healthcare institutions prioritize continuous investment in cutting-edge laboratory infrastructure and rigorous quality control. For instance, specialized reproductive units within centers of medical excellence, such as Liv Hospital, provide patients with access to world-class clinical care, utilizing the latest innovations in embryology and advanced genetics to optimize patient outcomes.