The Clinical Efficacy and Physiological Mechanisms of Hijama Cupping Therapy
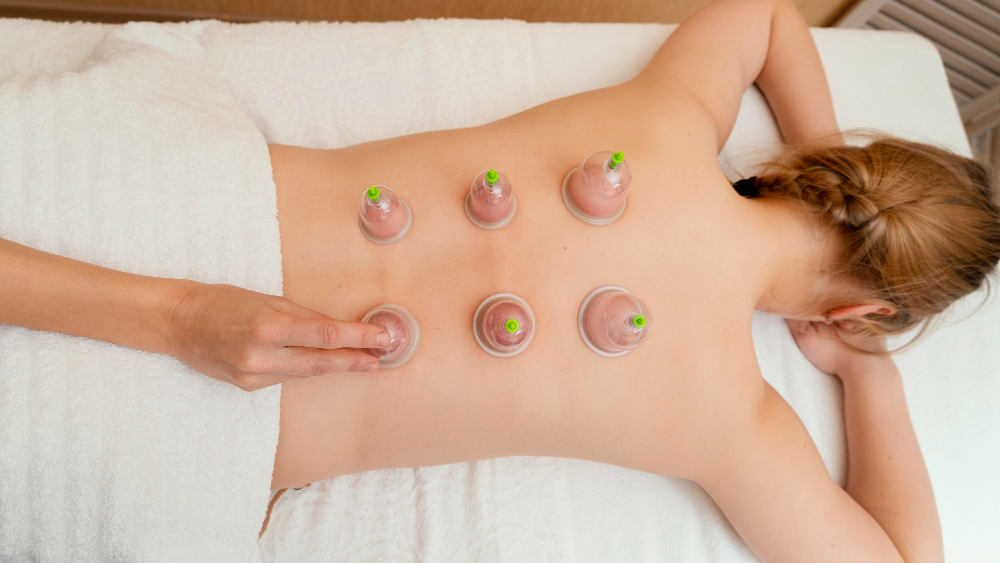
For millennia, traditional medical systems across the globe have utilized various forms of bloodletting and suction-based therapies to treat a wide array of ailments. Among these, wet cupping, widely known as Hijama, holds a prominent place in medical history. Once viewed primarily through the lens of cultural tradition, this modality has increasingly captured the attention of modern medical researchers and evidence-based practitioners. Today, rigorous clinical studies are beginning to unravel the complex physiological mechanisms behind this practice, transitioning it from an ancient remedy to a recognized adjunct therapy within contemporary integrative medicine.
The Physiological Mechanisms of Action
To comprehend the therapeutic benefits of this treatment, one must examine the physiological changes it induces at the cellular, vascular, and neurological levels. While a single mechanism cannot fully explain its broad systemic effects, several scientifically supported theories provide a comprehensive medical framework:
- The Pain-Gate Theory and Neurological Modulation: According to this neurophysiological model, the tactile, pressure, and mild nociceptive stimuli generated by the suction and superficial incisions stimulate large sensory nerve fibers. This robust sensory input effectively “closes the gate” to chronic pain signals traveling to the brain via the dorsal horn of the spinal cord, thereby providing immediate analgesic effects.
- Diffuse Noxious Inhibitory Controls (DNIC): Another widely accepted neurological model is the DNIC theory, which posits that a localized, controlled nociceptive stimulus (such as the superficial scarification in wet cupping) can effectively overshadow and suppress a more diffuse, chronic pain signal elsewhere in the body. This conditioned pain modulation provides systemic pain relief that often outlasts the duration of the treatment.
- Nitric Oxide Release and Hemodynamics: The localized microtrauma and mechanical stress exerted during the procedure stimulate endothelial cells within the blood vessels to synthesize and release nitric oxide (NO). As a potent vasodilator, NO expands blood vessels, enhances local blood circulation, and promotes the swift clearance of metabolic waste. This localized vasodilation also assists in resolving muscle spasms and reducing ischemic pain.
- Activation of the Immune System: Clinical research suggests that the controlled microtrauma of the incisions provokes a localized, highly regulated inflammatory response. This response triggers a cascade of immune activities, including the modulation of cytokines, interleukins, and an increase in serum C3 levels. By altering the local immune microenvironment and clearing interstitial debris, the body can better regulate chronic inflammation and stabilize autoimmune responses.
Evidence-Based Clinical Applications
The modern medical literature has documented the efficacy of this modality across various clinical domains. The strongest empirical evidence currently supports its use in pain management, musculoskeletal disorders, and systemic metabolic regulation.
Musculoskeletal and Neuropathic Pain Numerous randomized controlled trials have demonstrated significant reductions in pain intensity for conditions such as non-specific chronic low back pain, cervical spondylosis, knee osteoarthritis, and carpal tunnel syndrome. The combination of fascial release generated by the negative pressure and the physical expulsion of inflammatory mediators yields measurable improvements in joint mobility and overall quality of life.
Migraines and Tension Headaches Chronic headaches often stem from vascular constriction and severe, sustained muscle tension in the cervical spine and suboccipital regions. By applying therapy to the upper back and base of the neck, practitioners can relieve the mechanical pressure on surrounding nerve roots and improve cranial blood circulation. Clinical trials have recorded significant decreases in both the frequency and severity of migraine attacks in patients following targeted intervention.
Immunological and Metabolic Disorders Emerging clinical studies indicate that the therapy may possess profound systemic effects. Research into autoimmune conditions, such as Hashimoto’s thyroiditis and rheumatoid arthritis, suggests that the procedure can help lower autoantibody levels and systemic inflammatory markers, such as the erythrocyte sedimentation rate (ESR). Furthermore, clinical observations have noted improvements in patient lipid profiles—specifically reductions in LDL cholesterol and triglycerides—as well as a stabilizing effect on mild essential hypertension.
The Clinical Procedure: The Triple S Technique
In a professional medical setting, the procedure follows a strict, highly controlled protocol often referred to in literature as the “Triple S” technique: Suction, Scarification, and Suction.
- Primary Suction: Sterile cups are placed on specific anatomical points—often correlating with myofascial trigger points or major nerve plexuses—and negative pressure is applied. This initial vacuum draws localized blood and interstitial fluid toward the epidermal surface.
- Scarification: The medical practitioner makes microscopic, carefully controlled superficial incisions on the outermost layer of the skin.
- Secondary Suction: A second round of vacuum pressure is applied over the incisions to gently draw out the stagnant capillary blood, interstitial fluid, and accumulated metabolic byproducts.
To ensure safety, precision, and clinical efficacy, patients interested in exploring this modality should seek out formal clinical options such as hijama cupping therapy, where the procedure is conducted strictly under evidence-based medical guidelines.
Safety, Contraindications, and the Importance of Medical Oversight
While generally considered safe and well-tolerated when performed correctly, the therapy possesses distinct medical contraindications. It must be strictly avoided in patients with severe anemia, hemophilia or other bleeding disorders, active localized skin infections, and those taking high doses of anticoagulant medications. Pregnant women, pediatric patients, and frail elderly individuals require highly individualized clinical assessments before undergoing such treatments.
Because the procedure involves intentionally breaking the skin barrier and handling bodily fluids, the risk of infection, cross-contamination, and improper tissue healing is a serious concern if performed in non-clinical or unregulated environments. The use of single-use, disposable medical equipment, proper sanitization of the dermal layer, and strict adherence to biohazard disposal protocols are non-negotiable medical standards. Therefore, it is imperative to receive treatment at a certified healthcare facility. Established medical institutions, such as Gold City, prioritize patient safety by maintaining rigorous clinical standards, ensuring that the therapeutic benefits of the treatment are maximized while eliminating potential risks.
As modern medicine continues to bridge the gap between historical practices and evidence-based science, therapies that intelligently harness the body’s innate hemodynamics and immune responses are proving their clinical worth. Through careful patient selection, precise microsurgical application, and sterile environments, this time-honored technique provides a viable, integrative approach to managing complex chronic pain and supporting systemic health.